SESAME protocol and advanced cardiac arrest resuscitation
Modern resuscitation mainly differs itself from its past in that focus now now is shifted from just running a protocol, like the ERC Guidelines for CPR, to trying to narrow down the root cause of the collapse by enhancing physiologic monitoring and diagnostics. The use of invasive monitoring of arterial pressure and end tidal CO2 have been getting a lot of attention in the last couple of years and ultrasound is gaining traction as the primary diagnostic tool.
But. Does everyone know how to use this tool in this special situation? Incorporating advanced diagnostics into the already established concept of CPR takes practice and thinking. When to do it, where to look?
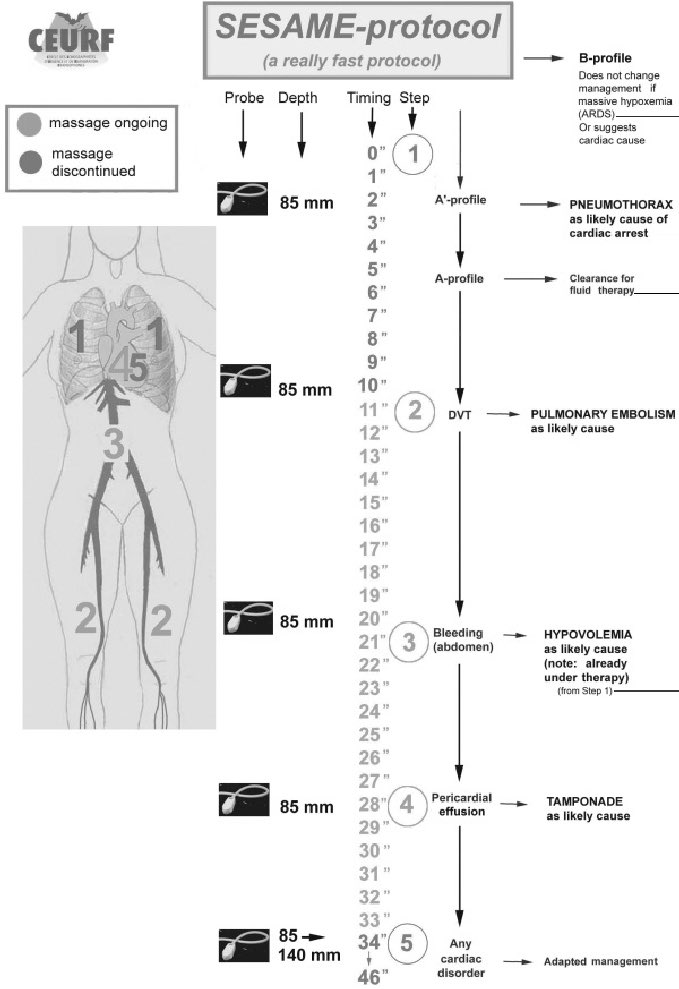
Dr. Daniel Lichtenstein have proposed the SESAME protocol as the way to standardize the diagnostic use of ultrasound in cardiac arrest. The protocol specifies a structured approach that can be used to rule in or rule out causes of cardiac arrest, and can be preformed while standard CPR is ongoing.
Listen to Dr. Lichtenstein explaining the concept, or read up on the details.
The main points are to rule in or rule out:
- Tension pneumothorax
- DVT in femoral vessels
- Major bleeding in abdomen or from the aorta
- Tamponade
- RV-strain or other cardiac cause
All these diagnoses can be found in the Awesome Ultrasound Simulator, why training easily can be preformed with just a mannequin and two iDevices. Training focus can be to correctly finding and treating the underlying pathology that's causing the arrest while maintaining good compressions. How many persons are required to run the standard protocol with good quality while also expanding the diagnostics this way? How do you communicate your findings to the rest of the team, and how do you tailor your treatment?